Injury recovery and physical rehabilitation is constantly changing. As the science improves and our understanding of human physiology deepens, we change our recommendations for injury recovery.
Bed rest used to be the standard treatment advice for acute low back pain. That was until we realized that early mobilization and activity dramatically improved the body’s ability to heal and regain function. [1]
Experiencing a sprained ankle playing pickleball is a relatively common injury on the pickleball court. This article will discuss why ankle sprains happen, how to treat an ankle sprain in the first 48-hours, how to rehab an ankle sprain in the first 2 to 6 weeks, and how to know when it is safe to return to play after a sprained ankle playing pickleball.
What is a sprained ankle?
“Acute ankle sprains are among the most common musculoskeletal injuries, and up to 70% of individuals who sustain an acute ankle sprain may develop residual physical disability, which may include chronic ankle instability.” [2]
An ankle sprain is a stretching or tearing of ligaments most often on the outside of the ankle. Ligaments connect bone to bone and provide stability to a joint (see also ‘Can Pickleball Help With Osteoporosis?‘).
Inversion Ankle Sprain
The most common sprained ankle playing pickleball is an inversion ankle sprain. Inversion is when the inner edge of the foot rolls up and the outer side of the ankle is overly stretched.
An inversion ankle sprain most often happens with a pickleball player’s body is moving laterally then tries to quickly change directions.
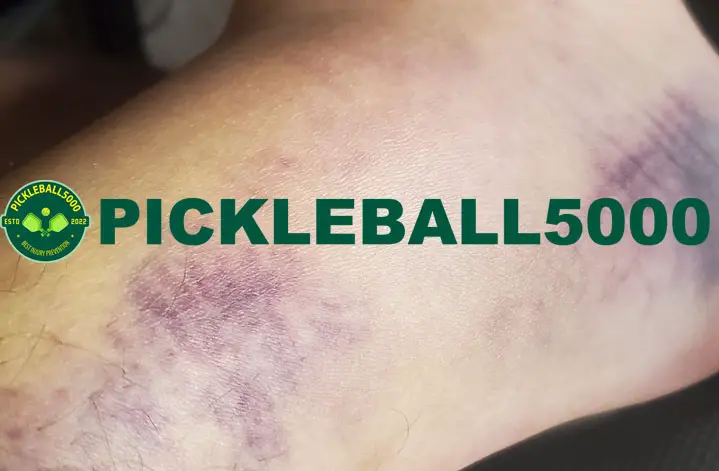
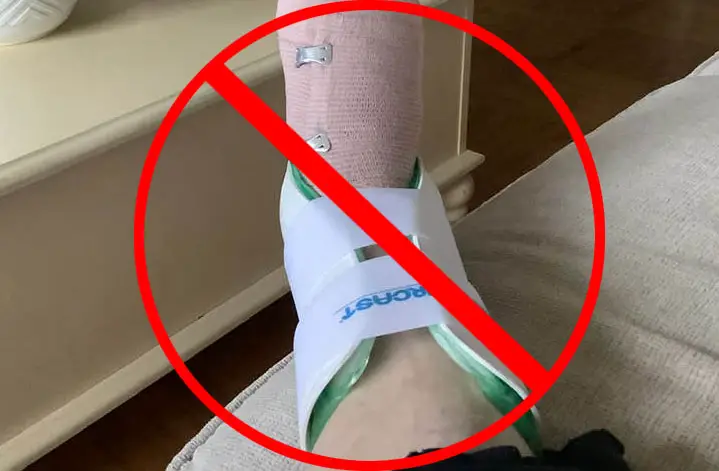
Why is it bad to immobilize a sprained ankle?
Acute ankle immobilization may help prevent further injury while the pickleball player is being transported to the medical professional for assessment. [3]
Immobilization of a pickleball ankle sprain longer than the time it takes for tranport to a medical professional and possibly x-ray to rule out bone fractures may result in longer than expected recovery times.
This article discusses early mobilization vs immobilization following an acute ankle sprain and does a great job sharing information from both sides.
Some of the cited problems with joint immobilization include:
- Weakening of ligament insertion sites
- Reduced load-to-failure
- Reduced energy-absorbing capacity of the bone-ligament-bone complex
- Collagen mass declines
- Collagen turnover increases with accelerated degradation and synthesis
Effectively, joint immobilization may cause more secondary impairments than controlled early mobilization and return to function. [4]
What is M.I.C.E – Pickleball Ankle Sprain
Movement – Immediately after a grade I or grade 2 ankle sprain, gentle range of motion will help faciliate fluid exchange, decrease tissue sensitivity, and assist lymphatic drainage.
Examples of early movement:
- Ankle pumps
- Toe Curls
- ABCs
Ice – While ice does not reduce inflammation or swelling as previously thought, ice is a great way to manage the pain experience. If you are someone who feels less pain when applying an ice pack to an injured area of the body, then ice is a safe and inexpensive way to reduce the subjective pain experience.
Compression – Using an ACE elastic bandage to provide a graded compression may be a great option to reduce acute swelling. A standard spiral wrap starting from the arch of your foot and progressing up around the ankle and lower leg will facilitate fluid removal, but it is important to note that compression for fluid removal is recommended for 10-minutes.
After 10-minutes the ace bandage should be removed to allow normalized blood flow and range of motion.
Compression may be combined with elevation to improve drainage.
Elevation – Elevation has been studied and shown to be most effective when the patient is laying flat on your back and your hip is flexed as close to 90-degrees as possible.
Sitting in a recliner or with your foot propped on a coffee table is not adequate elevation to reduce swelling.
Reference:
1. Rozenberg S, Delval C, Rezvani Y, Olivieri-Apicella N, Kuntz JL, Legrand E, Valat JP, Blotman F, Meadeb J, Rolland D, Hary S, Duplan B, Feldmann JL, Bourgeois P. Bed rest or normal activity for patients with acute low back pain: a randomized controlled trial. Spine (Phila Pa 1976). 2002 Jul 15;27(14):1487-93. doi: 10.1097/00007632-200207150-00002. PMID: 12131705.
2. Herzog MM, Kerr ZY, Marshall SW, Wikstrom EA. Epidemiology of Ankle Sprains and Chronic Ankle Instability. J Athl Train. 2019;54(6):603-610. doi:10.4085/1062-6050-447-17
3. DeYulis M, Hinson JW. Joint Immobilization. 2022 May 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 32491635.
4. Akeson WH, Amiel D, Abel MF, Garfin SR, Woo SL. Effects of immobilization on joints. Clin Orthop Relat Res. 1987 Jun;(219):28-37. PMID: 3581580.

